Convalescent plasma has been in the news a lot lately as a potential treatment for people infected with the coronavirus. In August the US Food and Drug Administration (FDA) granted emergency use authorization (EUA) to use these products based on preliminary data that suggested it might help people battling COVID. But there are still a lot of unanswered questions about this approach.
And that’s where you come in.
Plasma is a component of blood that carries proteins called antibodies that are usually involved in defending our bodies against viral infections. We also know that blood plasma from patients that have recovered from COVID-19, referred to as convalescent plasma, contain antibodies against the virus that can be used as a potential treatment for COVID-19.
That’s the theory, but the reality is that there are still a lot we don’t know, basic questions such as does it really work, how does it work, does it work for everyone or just some patients? A clinical grant includes testing the plasma in COVID-19 Positive patients that CIRM is funding with City of Hope, UC Irvine and Translational Genomics Research Institute (TGen) hopes to answer those questions.
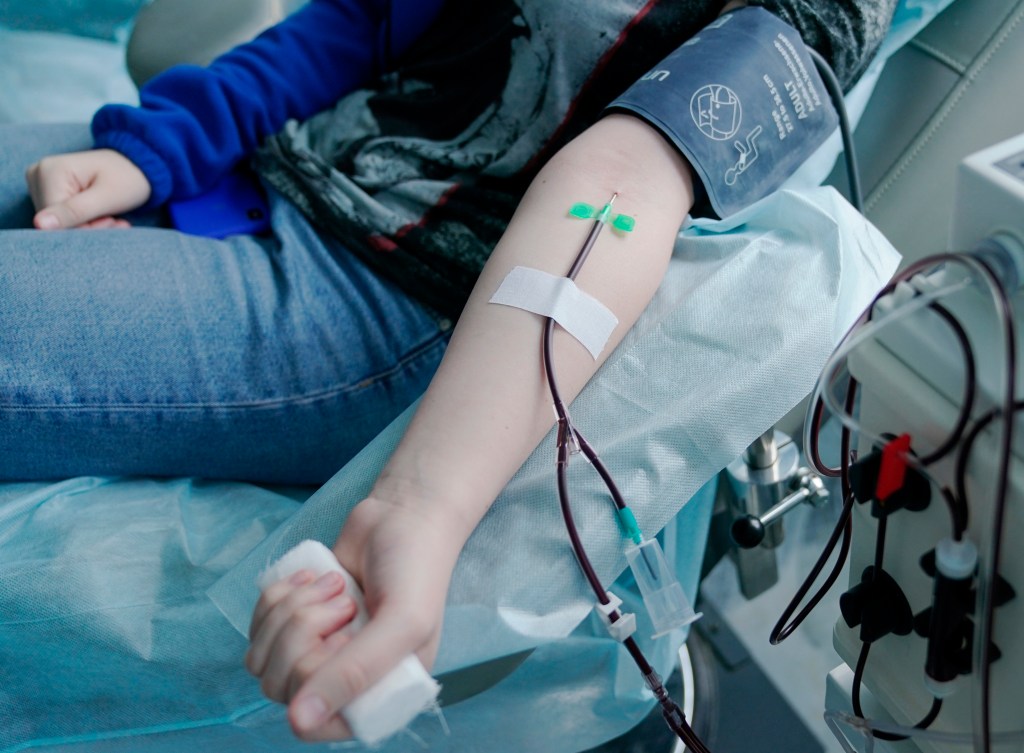
The first step is getting the plasma from people who have recovered from COVID and then testing it to make sure it’s safe and to identify what blood type it is, so you can match that blood type with the person receiving it.
But plasma doesn’t contain just one kind of antibody, there are many antibodies and each one works in a slightly different way. For example, two antibodies, IGM and IGG, target in on the spike protein on the coronavirus. The goal is to block that spike and prevent the virus from spreading throughout the body. IGM has up to 10 ‘arms’ and so has the potential to bind multiple copies of the spike, whereas IGG has only 2 arms, but lasts longer. Both IGM and IGG also come in many different flavors, allowing them to bind to many different parts of the spike, some being more protective than others.
That’s one of the things that this trial is trying to find out. And you can help them do that. The trial needs volunteers, volunteers to donate the plasma and volunteers to try the therapy.
The team is evaluating changes that occur before and after plasma treatment. Many recipients have no immediate response, a few get dramatically better, and some continue to have symptoms long after discharge from the hospital. These so-called “long-haulers” can have debilitating problems, months after becoming infected. The study hopes to evaluate these variable responses to plasma treatment.
But more people are needed if we are to truly understand what works best. We need people who are newly infected, those being treated with plasma, and those that have recovered from the virus.
We are particularly interested in recruiting people from the Black and Latinx communities, groups that are often underserved when it comes to access to medical care.
The team has created a website to make it easy to find out more about the clinical trial, and to see if you are a good candidate to be part of it, either as a donor or recipient.
Lives are at stake and time is short so join us, help us find answers to the most pressing medical issue of our times. It’s a chance to do something that might benefit your family, your friends and your community.
Since there is no effective vaccine and drugs are available, convalescent plasma is an alternative of choice to treat patients infected with Covid-19. There are 5 primary classes of immunoglobulin (Ig) available in blood and tissue fluids. These include IgG, IgM, IgA, IgD and IgE, which can be distinguished by the type of heavy chain found in the molecule Ig. When the pathogens enter and attack human body systems, the immune system is activated in response to foreign antigens. Macrophages and other killer cells move to the area of infection. Antigen-presenting cells such as macrophages and B lymphocytes destroy pathogenic antigen by process of phagocytosis and presented a tiny part of antigenic peptides in the form of MHC l and ll. This may activate proliferation and differentiation of lymphocytes into functional T killer cells and T helper cells. T helper cells recognize MHC-antigen complexes on the surface of B cells and promote the proliferation and maturation of antibody-producing B lymphocytes. However, clinical results are varying after Covid-19 infected patients treated with convalescent plasma. This is probably relying on plasma from donor who produces lg specific to certain epitope of antigen which may not compatible to the antigen from recipient. The genome of most viruses is not stable, the small changes of genetic sequence cause huge impact on specificity of Ig. Therefore, determination of virus strains in infected patients provide an important clues to develop an effective therapeutic treatment for Covid-19 infection.
Clinical finding showed that the existent of high levels of antibodies IgM and IgG in patients recovery from Covid-19 infection. In general, IgG is the most commonly found in human plasma and contain in largest amount. There are 4 subclasses of IgG with minor differences in its H chains but with distinct biological properties. The variety of IgG and complexity of biological responses in plasma of patients recovery from Covid-19 cause many different parts of spike are bound and varying degrees of protection in patients.
In normal subject, lgM is the first class of Ig produced by mature B cells and existence as antigen receptor on B cell surface. When IgM is secreted, the molecules appear as five of basic Y shaped units being joined together to make a large pentamer molecule with 10 antigen-binding sites. This large antibodies molecule is particularly effective at attaching to antigenic determinants present on the outer coats of miroganisms. The attachment of IgM may cause miroganism becoming agglutinate or clump together. Thus, IgM of patients recovery from Covid-19 showed up to 10 arms of molecules which are potentially bound to multiple copies of spike whereas IgG has only 2 arms.