By Kelly Shepard, PhD., CIRM’s Associate Director, Discovery & Translation
CIRM has previously blogged about advances in treating certain forms of “bubble baby” disease”, where a person is born with a defect in their blood forming stem cells that results in a deficient immune system, rendering them vulnerable to lethal infections by all manner of bacteria, virus or germ.
If a suitable donor can be found, or if the patient’s own defective cells can be corrected through gene therapy approaches, it is now possible to treat or cure such disorders through a bone marrow transplant. In this procedure, healthy blood stem cells are infused into the patient, taking up residence in his or her bone marrow and dividing to give rise to functioning immune cells such as T cells and B cells.
Unfortunately, there is another type of “bubble baby” disease that cannot be treated by providing healthy blood stem cells, because the defective immune system is caused by a different culprit altogether- a missing or dysfunctional thymus.
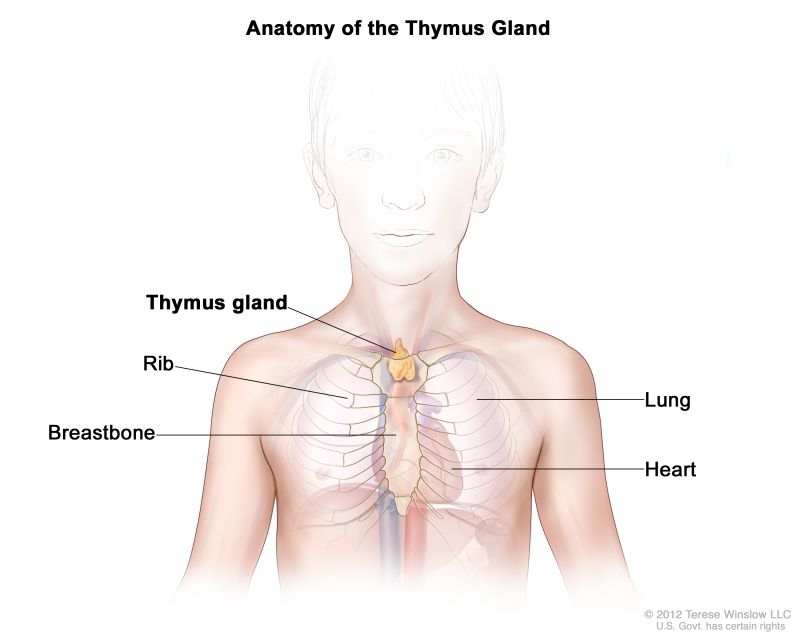
T Cells Go to School
What is a thymus? Most of us give little thought to this leaf-shaped organ, which is large and important in our early childhoods, but becomes small and inconspicuous as we age. This transformation belies the critical role a thymus plays in the development of our adaptive immune systems, which takes place in our youth: to prepare our bodies to fight infections for the rest of our lives.
One might think of the thymus as a “school”, where immature T cells go to “learn” how to recognize and attack foreign antigens (surface markers), such as those found on microorganisms or tissues from other individuals. The thymus also “teaches” our immune system to distinguish “self” from “other” by eliminating any T cells that attack our own tissues. Without this critical function, our immune system could inadvertently turn against us, causing serious autoimmune disorders such as ulcerative colitis and myasthenia gravis.
Many children with a severely deficient or absent thymus, referred to as athymia, have inherited a chromosome that is missing a key stretch of genes on a region called 22q11. Doctors believe perhaps 1/2000-1/4000 babies are born with some type of deletion in this region, which leads to a variable spectrum of disorders called 22q11 syndrome that can affect just about any part of the body, and can even cause learning disabilities and mental illness.
Individuals with one form of 22q11, called DiGeorge Syndrome, are particularly affected in the heart, thymus, and parathyroid glands. In the United States, about 20 infants are born per year with the “complete” and most severe form of DiGeorge Syndrome, who lack a thymus altogether, and have severely depressed numbers of T cells for fighting infections. Without medical intervention, this condition is usually fatal by 24 months of age.
Optimism and Setback
Although there are no therapies approved by the Food and Drug Administration (FDA) for pediatric athymia, Dr. Mary Louise Markert at Duke University and Enzyvant, Inc. have been pioneering an experimental approach to treat children with complete DiGeorge syndrome.
In this procedure, discarded thymic tissues are collected from infants undergoing cardiac surgery, where some of the thymus needs to be removed in order for the surgeon to gain access to the heart. These tissues are processed to remove potentially harmful donor T cells and then transplanted into the thigh of an athymic DiGeorge patient.
Results from early clinical trials seemed promising, with more than 70% of patients surviving, including several who are now ten years post-transplant. Based on those results, in June of 2019 Enzyvant applied to the FDA for a Biologics License Application (BLA), which is needed to be able to sell the therapy in the US. Unfortunately, only a few months later, Enzyvant announced that the FDA had declined to approve the BLA due to manufacturing concerns.
While it may be possible to address these issues in time, the need to step back to the drawing board was a devastating blow to the DiGeorge Community, who have waited decades for a promising treatment to emerge on the horizon.
New Opportunities
Despite the setback, there is reason to hope. In early 2019, CIRM granted a “Quest” Award to team of investigators at Stanford University to develop a novel stem cell based approach for treating thymic deficiency. Co-led by Katja Weinacht, a pediatric hematologist/oncologist, and Vittorio Sebastiano, a stem cell expert and developmental biologist, the team’s strategy is to coax induced pluripotent stem cells (iPS) in the laboratory to differentiate into thymic tissue, which could then be transplanted into patients using the route pioneered by Duke and Enzyvant.

The beauty of this new approach is that pluripotent stem cells are essentially immortal in culture, providing an inexhaustible supply of fresh thymic cells for transplant, thereby allowing greater control over the quality and consistency of donor tissues. A second major advantage is the possibility of using pluripotent cells from the patient him/herself as the source, which should be perfectly immune-matched and alleviate the risk of rejection and autoimmunity that comes with use of donated tissues.

Sounds easy, so what are the challenges? As with many regenerative medicine approaches, the key is getting a pluripotent stem cell to differentiate into the right type of cells in the lab, which is a very different environment than what cells experience naturally when they develop in the context of an embryo and womb, where many cells are interacting and providing complex, instructive cues to one another. The precise factors and timing all need to be worked out and in most cases, this is done with an incomplete knowledge of human development.
A second challenge relates to using cells from DiGeorge patients to produce thymic tissue, which are missing several genes on their 22nd chromosome and will likely require sophisticated genetic engineering to restore this ability.
Fortunately, Drs. Weinacht and Sebastiano are up to the challenge, and have already made progress in differentiating human induced pluripotent stem cells (iPS) into thymic lineage intermediates that appear to be expressing the right proteins at the right time. They plan to combine these cells with engineered materials to create a three-dimensional (3D) tissue that more closely resembles an authentic organ, and which can be tested for functionality in athymic mice.
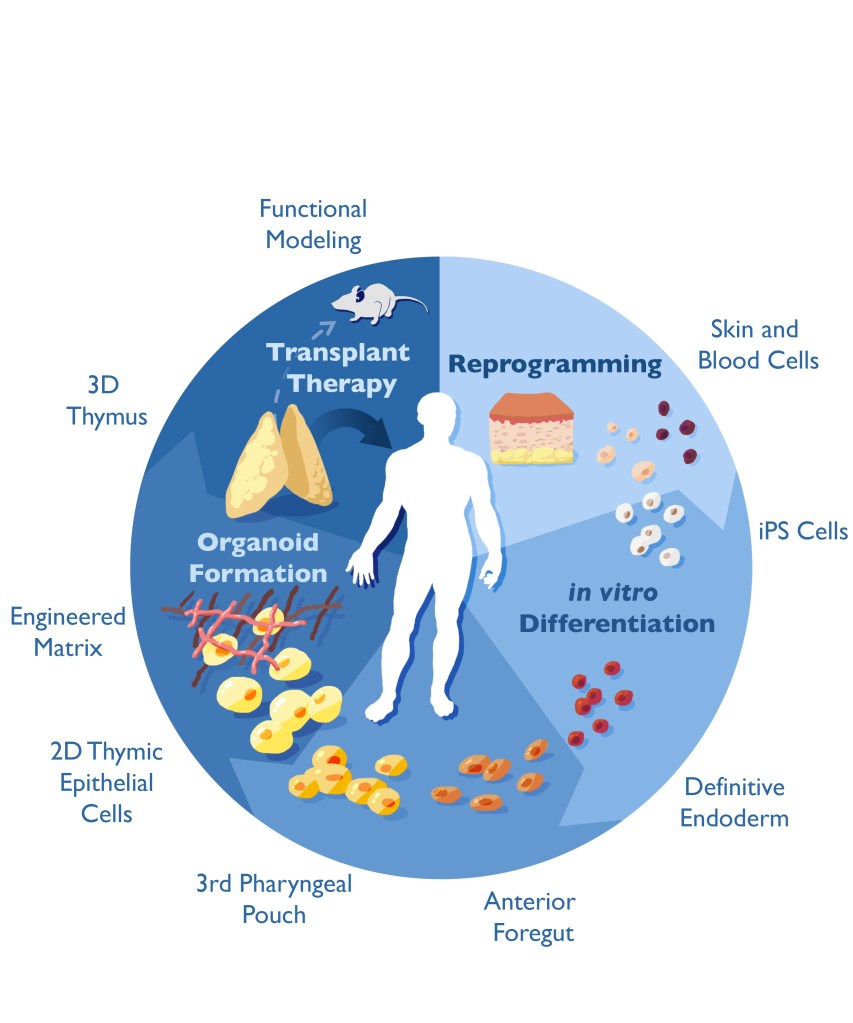
There is more work to be done, but these advances, along with continued technological improvements and renewed efforts from Enzyvant, could forge a path to the clinic and lead to a brighter future for patients suffering from congenital athymia and other forms of thymic dysfunction.
Any trials on stroke recovery going on????
Marie Frisch-koehler
Mc.fridch67@gmail.com