Ninety-five percent of all patients with chronic myeloid leukemia (CML), carry a Frankenstein-like gene, called BCR-ABL, created from an abnormal fusion of two genes normally found on two separate chromosomes. Like a water faucet without a shutoff valve, the resulting mutant protein is stuck in an “on” position and leads to uncontrolled cell division and eventually to CML as well as other blood cancers.
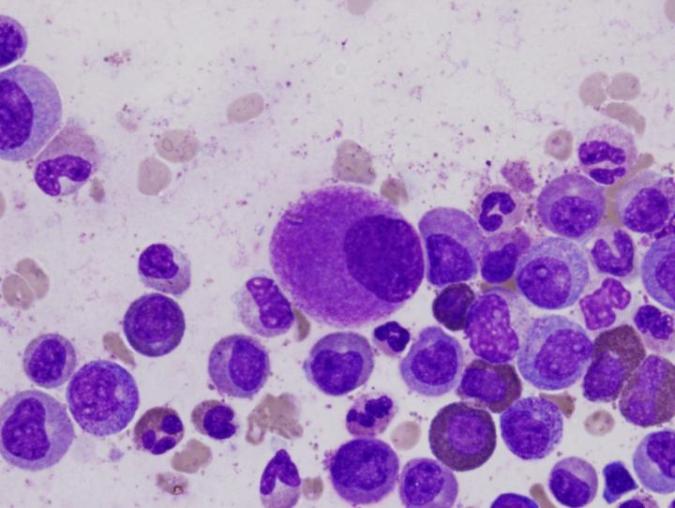
An oversized bone marrow cell, typical of chronic myeloid leukemia. Credit: Difu Wu
Gleevec, a revolutionary, targeted cancer drug that specifically blocks the BCR-ABL protein was approved by the FDA in 2001 and doubled 5-year survival rates for CML patients (31 to 59%) over that decade. Still, some patients who are responsive to the Gleevec class of drugs, become resistant to the treatment and suffer a relapse. Up until now, research studies pointed to an accumulation of additional DNA mutations as the driving force behind a rebound of the cancer cells.
But on Monday, a CIRM-funded UC San Diego team reported in PNAS that a reduction in just one protein, called MBNL3, in CML cancer cells activates a cascade of genes normally responsible for the unlimited self-renewing capacity of embryonic stem cells. Much like a researcher can reprogram a skin cell back into an embryonic like state via the induced pluripotent stem cell (iPSC) technique, this finding suggests that CML enhances its ability to spread by exploiting the same cellular reprogramming machinery.
CML is a slowly progressing cancer that initially begins with a chronic phase. At this stage, the cancerous cells, called blast cells, make up less than five percent of cells in the bone marrow. The phase usually lasts several years and is well controlled by drug treatment. A blast crisis phase follows when the blast cells make up 20 to 30% of the blood or bone marrow. At this stage, the patient’s condition deteriorates as symptoms like anemia and frequent infections worsen.
The UCSD team, led by Catriona Jamieson, director of Stem Cell Research at Moores Cancer Center, did a comparative analysis of CML patient samples and found that a reduction of MBNL3, a RNA binding protein, corresponded with CML progression from the chronic to blast phase. If you took intro biology in high school or college, you may recall that RNA acts as a messenger molecule critical to the translation of DNA’s genetic code into proteins. Some splicing and trimming of the RNA molecule occurs to prep it for this translation process. It turns out the decrease in MBNL3 in blast phase cells frees up stretches of RNA that leads to alternate splicing and, in turn, alternate forms of a given protein.
The study showed that in response to the decrease of MBNL3, an alternate form of the protein CD44, aptly named CD44 variant 3 (CD44v3), is increased in CML blast phase cells compared with chronic phase cells. Artificially over producing CD44v3 increased the activity of SOX2 and OCT4, two genes that are critical for maintaining the properties of embryonic stem cells. Genes involved with homing blood cells to the bone marrow were also upregulated.
Put together, these data suggest that this alternate RNA splicing not only helps CML blast phase cells preserve stem cell-like qualities, but it also helps sequester them in the bone marrow. Other studies have shown that the BCR-ABL protein inhibitor drugs are not effective in eradicating blast phase cells in the bone marrow, perhaps the reason behind relapse in some CML patients.
To try to smoke out these hiding blast phase cells in mouse CML studies, the team tested a combination treatment of a CD44 inhibitor along with the BCR-ABL inhibitor. While either treatment alone effectively removed the CML blast phase cells from the spleen and blood, only the combination significantly reduced survival of the cells in the bone marrow.
This tantalizing result has motivated the Jamieson team to pursue the clinical development of a CD44 blocking antibody with combination with the existing BCR-ABL inhibitors. As reported by Bradley Fikes in a San Diego Union Tribune story, the CD44 blocking antibody was not stable so more work is still needed to generate a new antibody.
But the goal remains the same as Jamieson mentions in a UCSD press release:
“If we target embryonic versions of proteins that are re-expressed by cancer, like CD44 variant 3, with specific antibodies together with tyrosine kinase [for example, BCR-ABL] inhibitors, we may be able to circumvent cancer relapse – a leading cause of cancer-related mortality.”