
The California Institute for Regenerative Medicine (CIRM) recently shared some encouraging news on The Stem Cellar about a CIRM-funded stem cell clinical trial for spina bifida at UC Davis Health.
Spina bifida is a birth defect that occurs when the spine and spinal cord don’t form properly and can result in life-long walking and mobility problems for the child, even paralysis.
Now, UC Davis has released more details about the clinical trial and the babies born after receiving the world’s first spina bifida treatment combining surgery with stem cells. The story was featured in BBC News and The Sacramento Bee.
The first phase of the trial is funded by a $9 million grant from the California Institute for Regenerative Medicine.
The one-of-a-kind treatment, delivered while a fetus is still developing in the mother’s womb, could improve outcomes for children with this birth defect.
A Decade’s Work
“I’ve been working toward this day for almost 25 years now,” said Dr. Diana Farmer, the world’s first woman fetal surgeon, professor and chair of surgery at UC Davis Health and principal investigator on the study.
In previous clinical trial, Farmer had helped to prove that fetal surgery reduced neurological deficits from spina bifida. Many children in that study showed improvement but still required wheelchairs or leg braces.

Farmer recruited bioengineer Dr. Aijun Wang to help take that work to the next level. Together, they researched and tested ways to use stem cells and bioengineering to advance the effectiveness and outcomes of the surgery.
Farmer, Wang and their research team have been working on their novel approach using stem cells in fetal surgery for more than 10 years. Over that time, animal modeling has shown it is capable of preventing the paralysis associated with spina bifida.
Preliminary work by Farmer and Wang proved that prenatal surgery combined with human placenta-derived mesenchymal stromal cells, held in place with a biomaterial scaffold to form a “patch,” helped lambs with spina bifida walk without noticeable disability. When the team refined their surgery and stem cells technique for canines, the treatment also improved the mobility of dogs with naturally occurring spina bifida.
The CuRe Trial
When Emily and her husband Harry learned that they would be first-time parents, they never expected any pregnancy complications. But the day that Emily learned that her developing child had spina bifida was also the day she first heard about the CuRe trial, as the clinical trial is known.
Participating in the trial would mean that she would need to temporarily move to Sacramento for the fetal surgery and then for weekly follow-up visits during her pregnancy.
After screenings, MRI scans and interviews, Emily received the news that she was accepted into the trial. Her fetal surgery was scheduled for July 12, 2021, at 25 weeks and five days gestation.
Farmer and Wang’s team manufactured clinical grade stem cells—mesenchymal stem cells—from placental tissue in the UC Davis Health’s CIRM-funded Institute for Regenerative Cures. The lab is a Good Manufacturing Practice (GMP) Laboratory for safe use in humans. It is here that they made the stem cell patch for Emily’s fetal surgery.
The Procedure
During Emily’s historic procedure, a small opening was made in her uterus and they floated the fetus up to that incision point so they could expose its spine and the spina bifida defect.
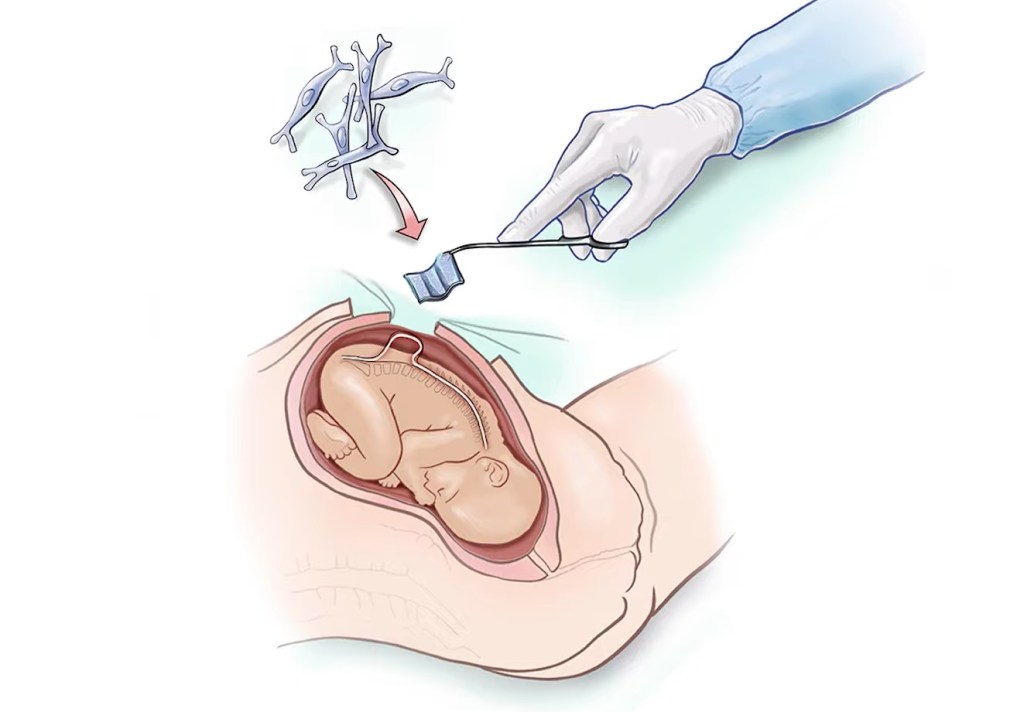
Then, the stem cell patch was placed directly over the exposed spinal cord of the fetus. The fetal surgeons then closed the incision to allow the tissue to regenerate. The team declared the first-of-its-kind surgery a success.
On Sept. 20, 2021, at 35 weeks and five days gestation, Robbie was born at 5 pounds, 10 ounces, 19 inches long via C-section.
For Farmer, this day is what she had long hoped for, and it came with surprises. If Robbie had remained untreated, she was expected to be born with leg paralysis.

“It was very clear the minute she was born that she was kicking her legs and I remember very clearly saying, ‘Oh my God, I think she’s wiggling her toes!’” said Farmer. “It was amazing. We kept saying, ‘Am I seeing that? Is that real?’”
Both mom and baby are at home and in good health. Robbie just celebrated her first birthday.

The CuRe team is cautious about drawing conclusions and says a lot is still to be learned during this safety phase of the trial. The team will continue to monitor Robbie and the other babies in the trial until they are 6 years old, with a key checkup happening at 30 months to see if they are walking and potty training.
“This experience has been larger than life and has exceeded every expectation. I hope this trial will enhance the quality of life for so many patients to come,” Emily said. “We are honored to be part of history in the making.”
Read the official release from UC Davis Health here.
There are many hormones play major roles during women pregnancy. These include : 1)Human chorionic gonadotropin hormone (hCG) which is produced in the placenta. 2)Human placenta lactogen (hPL) also known as human chorionic somatomammotropin is released in placenta. 3)Estrogen is produced in ovaries and placenta. It is important to maintain healthy pregnancy. 4)Progesterone is produced in ovaries and placenta during pregnancy. It stimulates thickening of the uterine lining for implantation of fertilized egg.
These hormones have important roles to induce growth factors for stem cells to growth and differentiate. Stem cells require growth factors for maturation into mature and functioning cells. Hence, different types of hormones are required to induce variety of growth factors for tissues and organs development. The lack of specific growth factor during fetus development may produce premature cells with partially function. These unhealthy cells with short lifespans may halt the fetus development. That was evidence in previous surgical and stem cells study showed that children have clinical improvement but some require wheelchair support and others with leg brace in their later of lives. To note that, application of stem cells to repair the deficiency of fetus development in certain stages of pregnancy is more efficient than child birth. As placenta is rich with variety of growth factors contributing many tissues and organs development in fetus. Therefore, growth factors research plays role to advance stem cells therapy for effective treatment of many human deficiency diseases.
Pingback: The Most Read Stem Cellar Blog Posts of 2022 | The Stem Cellar