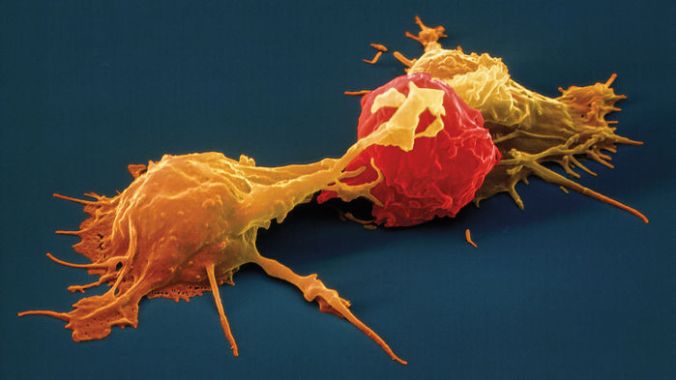
Stem cell image of the week: Our stem cell image of the week shows natural killer cells (yellow) attacking a cancer cell (red).
The cancer fighters known as CAR T cells have proved their prowess in recent years. Three therapies using the altered T cells against lymphoma or leukemia have won U.S. Food and Drug Administration approval, and hundreds of trials are now unleashing them on other malignancies, including solid tumors. But the cells may soon have company. Researchers have equipped other immune guardians—natural killer cells and macrophages—with the same type of cancer-homing receptor, and the natural killer cells have made their debut in clinical trials.
CAR T cells—their name comes from the chimeric antigen receptor, or CAR, added to help the immune cells target cancer cells—inspired the new work. CAR natural killer (CAR NK) cells could be safer, faster to produce, and cheaper, and they may work in situations where T cells falter. CAR-carrying macrophages also have potential advantages, and one firm plans to launch the first clinical trials of these cells next year.
Although they aren’t likely to replace CAR T cells, these alternative cancer fighters “could be an addition to the armamentarium of cell therapies,” says hematologist and oncologist Katy Rezvani of the University of Texas MD Anderson Cancer Center in Houston. She is leading the first trial of CAR NK cells in the United States, which began in 2017, and organizing another that is due to start this year.
“Natural killer cells are our first line of defense against cancer cells,” Rezvani says. They scan other cells in the body and destroy any that are infected or otherwise abnormal, including tumor cells. Researchers have been trying to harness the cancer-fighting activity of NK cells that don’t carry CARs for more than 20 years, notes translational immunologist Jeffrey Miller of the University of Minnesota in Minneapolis. But upgrading them by adding CARs seems to boost their potency.
CIRM-funded spinal cord injury trial produces more encouraging results (Kevin McCormack)
Way back in 2010 Geron became the first ever company to get approval from the Food and Drug Administration (FDA) to carry out a clinical trial using embryonic stem cells to treat people with spinal cord injury. CIRM funded that work and even though the company later halted the trial (for business reasons) it was a small piece of stem cell history.
Fast forward eight years and Asterias Biotherapeutics has taken up where Geron left off, using the same approach. This week Asterias published the latest results from its CIRM-funded clinical trial and they are encouraging.
They have done 24-month follow-ups on six patients (including Jake Javier and Chris Boesen who we have blogged about) who received 10 million cells transplanted into their spine. None experienced any serious side effects and MRI examinations showed evidence that the stem cells had engrafted at the injury site in all six patients. Often after a spinal cord injury a cavity can form at the injury site and scar tissue or fill up with fluid, preventing the spinal cord from healing. The evidence of engraftment means there is no such cavity.
Even more encouragingly all six have recovered at least one motor level (a measure of how much movement or function they have regained) on at least one side and five have recovered two or more motor levels on at least one side.
This kind of recovery can make the difference between needing round-the-clock care and being able to lead an independent life.
In a news release, Ed Wirth, the Chief Medical Officer at Asterias, said this shows the benefits of the therapy appear to be long-lasting:
“While the primary endpoint for the SCiStar trial was 12 months, we are further encouraged by this additional follow-up data that shows both durable engraftment and motor function recovery being maintained or improved upon at 24 months.”
The company hopes to meet with the FDA later this year to plan for a future trial of the therapy.
Planaria Worm Their Way into Human Stem Cell-Related Research (Todd Dubnicoff)
The planaria flatworm has astounding regenerative capabilities. Cut it in half and the missing side grows back. Decapitate it and the head grows back in about two weeks. Many researchers are eager to unlock the cellular and molecular mechanisms of planaria’s seemingly supernatural powers in order to bestow them onto humans suffering from disease or injury. But humans and worms are so different, how could you ever make any meaningful connections between the species?
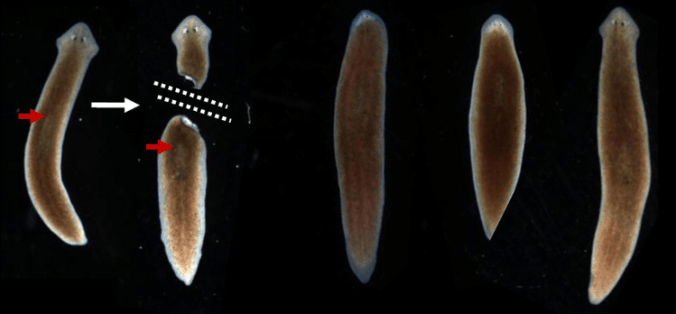
Decapitated planaria regrows head within a couple of weeks. Photo credit: Michael Levin And Tal Shomrat, Tufts University
Well, in a report published this week, Oxford University researchers found that planaria have more in common with humans than was previously thought when it comes to the way both species regulate gene activity in stem cells. These findings make these worms an even more valid model system for exploring novel therapeutic strategies for people.
Up until this study, it was thought that only vertebrates (animals with back bones like mammals, birds and fish) use a mechanism called bivalency in their stem cells to maintain the ability to specialize into different types of cells. With bivalency, a subset of genes within stem cells are neither turned off nor turned on. Instead they’re in a “poised” state, ready to be silenced or activated depending on the eventual fate of that particular cell.
By studying the chemical modifications of DNA, called epigenetics, that play a role in gene activity and bivalency, the research team showed that bivalency is also employed by planaria, a simple invertebrate. Professor Aziz Aboobaker, the lead author on the study, explained the significance of this finding in a press release:
“The results of this approach served to confirm the team’s findings that bivalency seems likely to have evolved earlier in multicellular animal evolution than we thought, and this adds to the growing narrative that simple worm stem cells and our stem cells have much more in common then we imagined when we started this work.”
This commonality makes the easy-to-study planaria an attractive model system to study given that dysfunctions in these chemical modifications of DNA have been linked to human disease.
The study is published in Genome Research.