 |
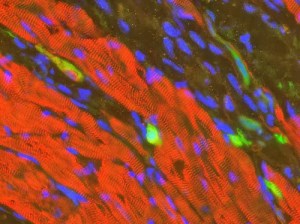
| Heart muscle cell made from reprogrammed skin cells |
“Six year old Sierra Bingham had the flu.” It’s a simple opening line to a story that quickly takes on a nightmarish twist. It’s about an Oregon family with four children. Because of a hereditary condition two of those children ended up getting heart transplants, and a third got an implantable device to support his heart.
The article is the cover story for the latest issue of Stanford Medicine magazine, a fascinating look at the terrible toll heart disease has in this country, and the potential for stem cells to treat those problems.
As the article succinctly states:
“It’s not a pipe dream. The California Institute for Regenerative Medicine has doled out over $120 million to hasten potential therapies into clinical trials — including $20 million to Wu and Deepak Srivastava, MD, director of cardiovascular and stem cell research at the Gladstone Institutes in San Francisco. And in January 2014, big pharma stepped up with a $12.5 million investment from Johnson & Johnson in Los Angeles-based Capricor Therapeutics Inc. to investigate whether cardiac stem cells can repair heart attack damage.”
The Wu in question is Dr. Joseph Wu, M.D., Ph.D., director of the Stanford Cardiovascular Institute. He is using human embryonic stem cells to create heart muscle cells called cardiomyocytes and see if they can help end stage heart failure patients.
Wu also talks about the potential for induced pluripotent stem cells to be used to screen medications and to personalize treatment.
“This will be the personalized medicine of the future,” says Wu. “Instead of giving a drug to 5,000 patients as part of a clinical trial, we can test the drug in the laboratory on iPS-derived beating heart cells from patients — a kind of clinical trial in a dish. And, if you have heart disease, we’ll be able to test potential drug therapies on your cells rather than using you as a guinea pig as we try to figure out what works best.”
It’s a wonderfully in-depth article about the potential of stem cells to save the lives of people with end stage heart failure. It’s also a reminder that for families like the Binghams this is personal, and that without these therapies their children may face a very uncertain future.
kevin mccormack